
Trophectoderm embryo biopsy is also called day 5 biopsy
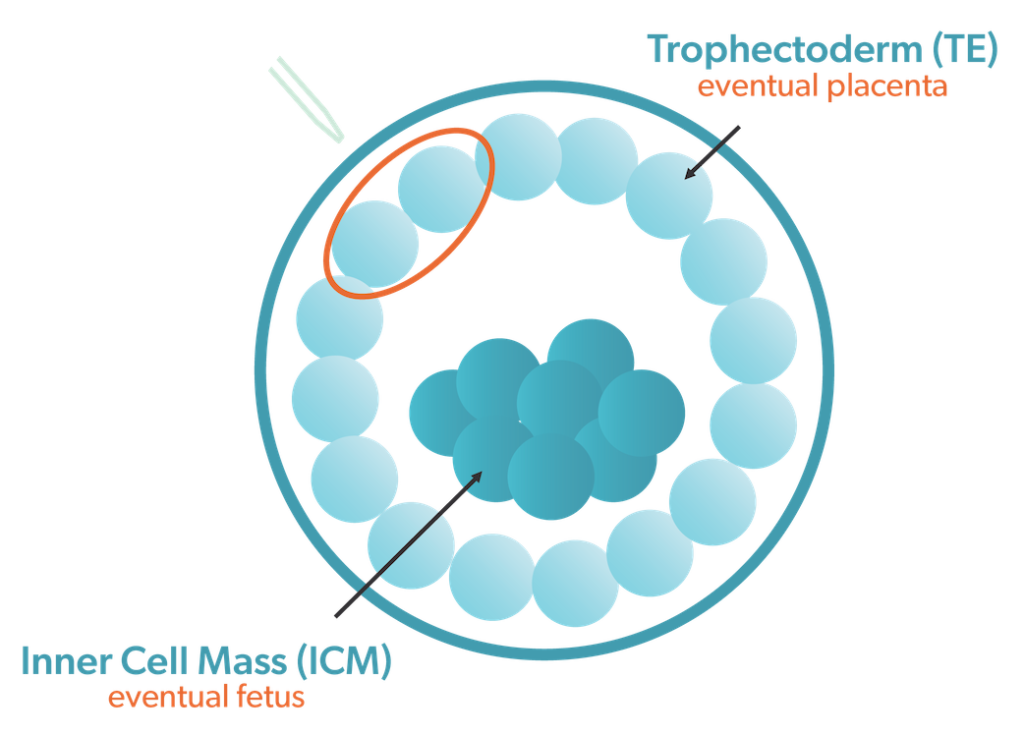
When embryos are biopsied on Day 5 of live, a few cells (usually 4 or 5) is removed from the trophectoderm of an embryo in a blastocyst stage. A blastocyst embryo has 2 different types of cells, the inner cell mass (ICM) and the trophectoderm. The ICM will become fetus while the trophectoderm becomes the placenta.
 During the biopsy, a laser is used to open a small window in the shell of the embryo (called the zona pellucida).
During the biopsy, a laser is used to open a small window in the shell of the embryo (called the zona pellucida).
Then a few cells are removed from the embryo, the part of the embryo that becomes the placenta. These cells are removed with very small instruments connected to a microscope. Because a blastocyst is made up of 100 or more cells, removing a few cells from the trophectoderm does not impair the embryo’s ability to continue to develop. Embryos develop at different rates, so in our lab, they are biopsied on day 5, 6 or 7 – whenever the embryo develops into a blastocyst.
After the biopsy, the embryos are vitrified which is a process of quick freezing.
The cells that were removed are shipped to a testing laboratory. San Antonio IVF lab receives the results of the testing and the patient is informed of the results. Then, a frozen embryo transfer cycle is begun. Typically, one normal embryo is thawed and transferred to the uterus after preparation with estrogen and progesterone.
Day 5 biopsy, or trophectoderm biopsy is better tolerated by embryos than a biopsy done on day 3. Also, the results of the biopsy may be more accurate due to something called mosaicism. When the embryo has only 6-8 cells (typical for a day 3 embryo), sometimes there are cells in the embryo that are different chromosomally than the other cells. The theory is that abnormal cells can be excluded as the embryo develops. The risk of mosaicism resulting in false biopsy results is lower when the embryo has reached the blastocyst stage, partly because more than one cell can be removed from the embryo.
Trophectoderm biopsy is most commonly done for preimplantation genetic screening (PGS).
PGS tests the embryos to determine the number of chromosomes present in the cells of the embryo. Embryos should have 46 chromosomes, one copy of each autosome and either two X chromosomes (female) or an X and a Y chromosome (male). If the embryo has an abnormal number of chromosomes, it will typically fail to implant and the pregnancy test will be negative. Alternatively, these embryos usually result in miscarriage. Only embryos that are consistent with live (viable) are considered for transfer to the uterus. The other kind of testing that can be done after trophectoderm biosy is preimplantation genetic diagnosis (PGD). PGD is done to determine if embryos carry specific diseases such as Spinal Muscular Atrophy or Tay Sachs Disease.



